Surgical procedures often involve prolonged immobility, which can increase the risk of developing common complications such as deep vein thrombosis (DVT) and pulmonary embolism (PE). To mitigate these risks, medical professionals frequently utilize intermittent pneumatic compression (IPC) devices. IPC devices have been proven to reduce and prevent blood clotting during and after surgery. In this article, we explore the reasons why IPC devices are an integral part of surgical care, their mechanism of action, and the benefits they offer.
Reducing the Risk of DVT & PE
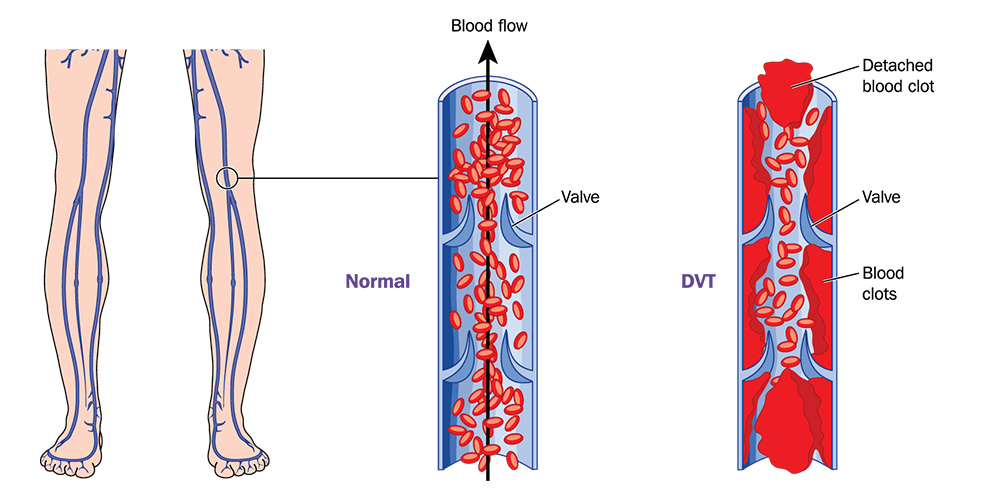
DVT occurs when blood clots form in the deep veins of the legs, while PE involves the migration of these clots to the lungs. Both conditions can have severe consequences, leading to morbidity and mortality. During surgeries, patients may experience reduced blood flow and slower circulation due to sedation, immobility, and prolonged exposure to anesthesia. To counteract these effects, IPC devices are used to facilitate blood flow, preventing the formation of blood clots and reducing the likelihood of DVT and PE.
How IPC Devices Work
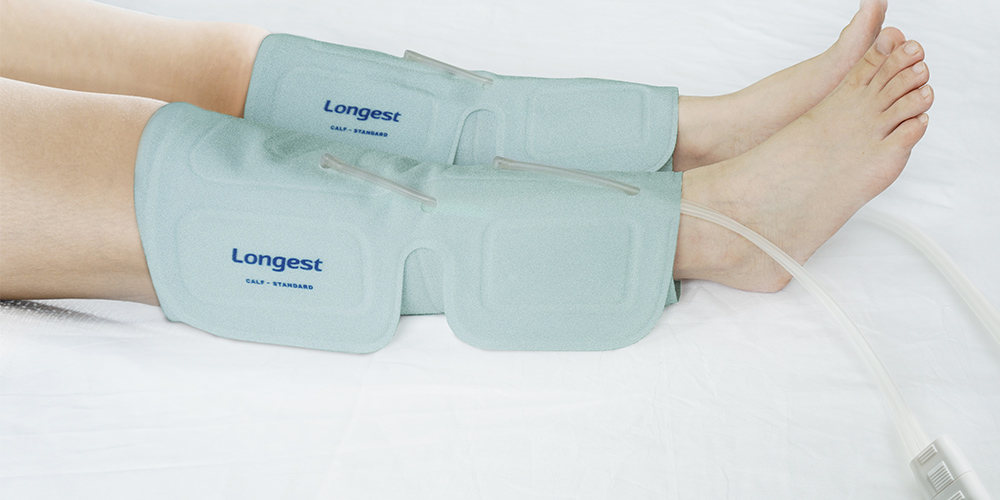
IPC devices comprise inflatable sleeves that are wrapped around the patient's legs or lower extremities. These sleeves are connected to an air pump, which periodically inflates and deflates the compartments, applying pressure on the veins. The alternating compression and release simulate the natural muscular contractions that occur during walking, thereby activating the calf muscle pump to propel blood back toward the heart.
Benefits of Using IPC Devices
1. Prevention of Deep Vein Thrombosis: IPC devices significantly reduce the risk of developing DVT by increasing blood flow and preventing stasis in the lower extremities. By gently compressing the veins, these devices facilitate the removal of waste products and prevent the accumulation of clots, safeguarding patients from potentially life-threatening conditions.
2. Enhanced Circulation: Prolonged periods of immobility can hamper blood circulation in surgical patients, leading to edema (swelling) and impaired tissue perfusion. IPC devices improve circulation by increasing venous return, thereby enhancing oxygen and nutrient delivery to tissues. This aids in the reduction of postoperative swelling and promotes faster healing.
3. Decreased Hospital Stay and Costs: By using IPC devices, patients experience fewer postoperative complications such as DVT and PE. By mitigating these risks, the need for extended hospitalization and additional treatments can be reduced, resulting in shorter hospital stays and decreased healthcare costs.
4. Nonpharmacological Intervention: IPC devices offer a non-invasive and nonpharmacological approach to preventing DVT and promoting blood circulation. This makes them suitable for patients with contraindications or allergies to certain medications, as well as those who prefer to minimize the use of drugs whenever possible.
In conclusion, IPC devices are valuable tools in the prevention of postoperative complications, particularly DVT and PE. By enhancing blood flow, reducing stasis, and facilitating the calf muscle pump mechanism, IPC devices effectively reduce the risk of clot formation and improve circulation. When used during surgeries, these devices contribute to shorter hospital stays, reduced healthcare costs, enhanced patient outcomes, and improved overall patient safety. As medical advancements continue, coupled with the growing recognition of patient care, the use of IPC devices is expected to become even more widespread in surgical settings.
Advanced IPC device for DVT Prevention
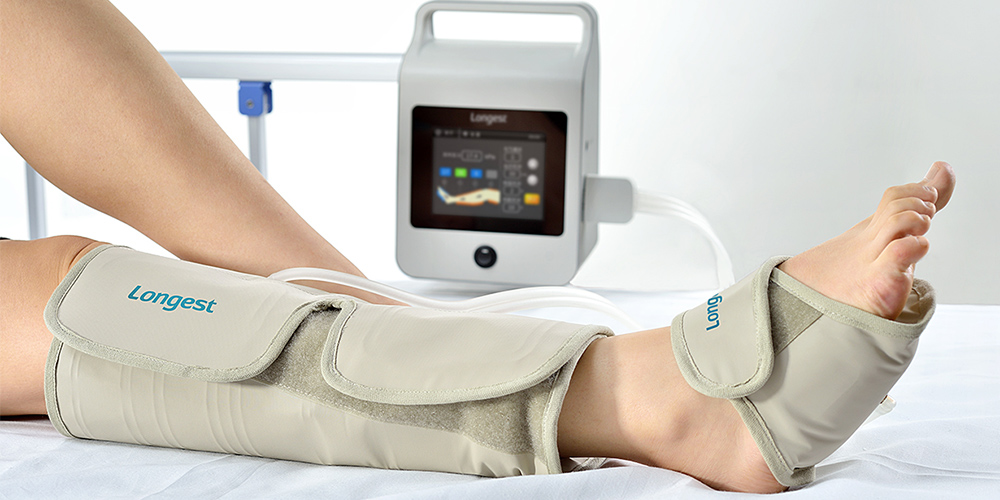
The outstanding IPC device LGT-2200DVT is designed to make DVT prevention in hospital settings more convenient and more efficient. The device is remarkably compact in dimensions and lightweight, making the daily transport and usage of the device more convenient. Besides AC Power, the device can be powered by a rechargeable battery with over a 4-hour battery life, reducing the use of cords in the patient room to improve patient safety.
Despite its small size, it delivers impressive functionality with a high-performance pump and comprehensive compression sleeve options. A wide range of pressure allows us to meet more clinical needs and the comfort levels of different patients, improving clinical versatility and patient experience.
The LGT-2200DVT is a durable and reliable helper for healthcare givers in everyday DVT prevention work. It provides effective DVT prevention and management while ensuring patient safety and comfort.
About Longest Medical
Longest Medical has been committed to the development and manufacturing of advanced and reliable rehabilitation devices since 2000. The provide a wide range of rehabilitation products including IPC devices & sleeves for DVT prevention. Various models of DVT pumps that are user-friendly, lightweight, and portable are available.